I am very lucky in that neither my mom, nor I, suffer from diabetes, although that is not to say that my mom doesn’t have the necessary health checks for it. That doesn’t mean, though, that you don’t need to know for your loved ones, the Medicare coverage, and guidelines, for diabetes, and so I am writing a series of at least three posts to help with that.
Medicare Part B covers diabetic shoes, inserts and in some cases molded shoes, if you qualify under the Medicare guidelines.
- you have to have a diagnosis and certification from your physician that you have diabetes – this has to be from the physician who is actually personally managing your systemic diabetes condition and that you have diabetes mellitus
- the/your physician must also certify that you are being “treated under a comprehensive diabetes care plan and need therapeutic shoes and/or inserts because of diabetes”
- your physician must certify that you have one or more, of a number of foot conditions, in one or both feet
Note, that your physician who is treating you for diabetes, and giving all the certifications, must be a Medicare-enrolled physician, or you will not qualify for Medicare coverage.
The document the physician is providing is called a Statement of Certifying Physician, and only the treating physician can complete and then sign this document.
The Certifying Physician must be an M.D. or D.O., and may not be a podiatrist, physician assistant, nurse practitioner, or clinical nurse specialist.
A nurse practitioner or physician assistant cannot complete the document and then have the physician sigh it, it must all be written and signed by the treating physician.
The following are the foot conditions, one of which you must have to qualify for coverage from Medicare Part B –
- Complete partial foot amputation
- Past foot ulcers
- Calluses that could lead to foot ulcers
- Nerve damage because of diabetes with signs of problems with calluses
- Poor circulation
- A deformed foot
The source of the list of foot conditions is “Medicare Coverage of Diabetes Supplies, Services, & Prevention Programs” which you can read or download here.
The Certifying Physician can either delegate the documentation of the qualifying foot condition to a podiatrist, other M.D. or D.O., physician assistant, nurse practitioner or clinical nurse specialist, or conduct the foot examination themselves.
Contents Overview & Quicklinks
Who prescribes the shoes and inserts ?
What about the provider/supplier ?
About the supplier and “assignment”
Let’s round that up in an easy set of steps
To find a supplier/qualified provider for your shoes and inserts
What type of shoes and inserts does Medicare give coverage to ?
How much coverage does Medicare give to therapeutic shoes and inserts for diabetes ?
Medicare diabetic shoes near me ?
What equipment does Medicare cover ?
How do you get coverage from Medicare Part B for DME ?
Medicare-enrolled DME Supplier near me ?
What about Medicare Advantage ?
List of Durable Medical Equipment generally covered by Medicare
Free one-on-one help with understanding Medicare
If I don’t have Medicare, what about Medicaid ?
How to find the HCBS programs, waivers and 1915 waivers in your state ?
If your income is a bit too high to qualify for Medicaid
Does Tricare cover therapeutic shoes and inserts for Veterans ?
Does ChampVA cover therapeutic shoes and inserts for veterans ?
Who prescribes the shoes and inserts ?
The shoes and inserts must be prescribed by a Podiatrist (The Prescribing Practitioner), which is a foot doctor, or other qualified healthcare provider – these may be a physician assistant, nurse practitioner, or clinical nurse specialist.
Once you have the Statement of Certifying Physician from the physician who is treating you for diabetes, you then need to see a podiatrist or other qualified health care provider for the correct prescription.
The Prescribing Practitioner is the one who will write the order for the therapeutic shoes, modifications and inserts.
Again, please remember that the Prescribing Practitioner – the Podiatrist, or other qualified healthcare provider, who gives you the prescription for the shoes and inserts must be Medicare-enrolled, otherwise you will not receive your Medicare coverage.
What about the provider/supplier ?
The shoes must be provided by –
“A doctor or other qualified individual like a pedorthist, orthotist, or prosthetist fits and provides the shoes.”
The source of the text is again “Medicare Coverage of Diabetes Supplies, Services, & Prevention Programs” which you can read or download here.
The podiatrist, or qualified healthcare provider (The Prescribing Practitioner), who prescribed your therapeutic shoes, modifications and inserts may also be the supplier.
About the supplier and “assignment”
You must make sure that the supplier, who will be from one of the listed professions above, is Medicare-enrolled, and that they are a “participating” supplier.
If they are not Medicare-enrolled, you will not receive coverage.
If they are not a “participating” supplier this means they do not accept assignment, which is the Medicare-approved price, and can charge much more than a “participating” supplier who accepts assignment, so do verify that with them.
Let’s round that up in an easy set of steps
Step 1
You need all the paperwork from the physician who is treating you for diabetes (the certifying physician), which must contain –
- the diagnosis of diabetes mellitus
- the results of the foot condition examination
- the certification that you are being treated under a comprehensive diabetes care plan
- and that you therapeutic shoes and inserts because of diabetes
Step 2
Next you see the podiatrist (Prescribing Practitioner), or other qualified healthcare provider – as outlined above – for an in-person consultation for the prescription for the shoes.
Step 3
Your prescription now has to be filled by a Medicare-enrolled Supplier.
In the case of therapeutic shoes and inserts, the supplier can be –
- the person who prescribed your shoes (Prescribing Practitioner)
or
the supplier can be any one of the following qualified providers –
- a podiatrist
- a pedorthist
- an orthotist
- a prosthetist
To find a supplier/qualified provider for your shoes and inserts
If your treating physician doesn’t point you in the right direction, here are some tools to locate qualified providers/suppliers for your shoes and inserts.
To find a Podiatrist – you can use the locator tool on the American Podiatric Medical Association website here.
To find a Pedorthist – you can use the locator tool on the Pedorthic Footcare Association website here.
To find a Prosthetist – you can use the locator tool on the Prosthetist Finder website here.
To find an Orthotist – you can use the locator tool on the American Board for Certification in Orthotics, Prosthetics and Pedorthics here.
Obviously, you can use the last locator to find Pedorthists and Prosthetists as well as Orthotists.
Remember to only use Medicare-approved suppliers and those who accept assignment !
What type of shoes and inserts does Medicare give coverage to ?
If you have Medicare Part B and you have met all the Medicare conditions to qualify for shoes and inserts for diabetes,
“The types of shoes that are covered each year include one of these:
- One pair of depth-inlay shoes and 3 pairs of inserts
- One pair of custom-molded shoes (including inserts) if you can’t wear depth-inlay shoes because of deformity, and 2 additional pairs of inserts
Note: In certain cases, Medicare may also cover separate inserts or shoe modifications instead of inserts.”
The source of the text is again “Medicare Coverage of Diabetes Supplies, Services, & Prevention Programs” which you can read or download here.
How much coverage does Medicare give to therapeutic shoes and inserts for diabetes ?
Typically, Medicare will give 80% coverage to the Medicare-approved cost of therapeutic shoes and inserts for diabetes, leaving you cover the 20% coinsurance of the Medicare-approved cost.
This is of course if you used all Medicare-enrolled doctors, providers and suppliers, and a supplier who was a Medicare-enrolled “participating” supplier who accepts assignment.
On the point of payment, Medicare advices the following –
“To find out how much your test, item, or service will cost, talk to your doctor or health care provider. The specific amount you’ll owe may depend on several things, like:
- Other insurance you may have
- How much your doctor charges
- Whether your doctor accepts assignment
- The type of facility
- Where you get your test, item, or service”
The source of the text is Medicare’s website page on coverage for therapeutic shoes, which you can read here.
With regard to the doctors, providers and suppliers for therapeutic shoes, Medicare also writes –
“Medicare will only cover your therapeutic shoes if your doctors and suppliers are enrolled in Medicare. Doctors and suppliers have to meet strict standards to enroll and stay enrolled in Medicare. If your doctors or suppliers aren’t enrolled, Medicare won’t pay the claims submitted by them.
It’s also important to ask your suppliers if they participate in Medicare before you get therapeutic shoes. If suppliers are participating suppliers, they must accept assignment. If suppliers are enrolled in Medicare but aren’t “participating,” they may choose not to accept assignment. If suppliers don’t accept assignment, there’s no limit on the amount they can charge you.”
The source of the text is Medicare’s website page on coverage for therapeutic shoes which you can read here.
Medicare diabetic shoes near me ?
Typically, when you are getting the shoes made and fitted, the provider/supplier, who will be a Podiatrist, Pedorthist, Orthotist or Prosthetist, will already have brands and types of shoes and inserts they work with, that they will recommend.
If you have a specific brand of shoe that you would like, you are going to have to find someone who works with that brand.
For the brand Dr. Comfort, you can go to their website and use a locator to find all the foot specialists who work with their brand and are providers/suppliers, and who can fill your prescription with a Dr Comfort shoe.
The Dr Comfort locator can be found here.
Don’t forget to make sure they are Medicare-approved.
What equipment does Medicare cover ?
The type equipment that Medicare covers for use in the home is called “durable medical equipment”, or DME.
For an item of medical equipment, or of medical supplies, to qualify as durable medical equipment it must –
- be able to withstand repeated use over a period of time – durable
- be for a medical reason only – not for comfort
- useful to someone who is actually sick, and of little use to a person who is well
- be primary for use in the home
- have a lifetime of at least 3 years
How do you get coverage from Medicare Part B for DME ?
To qualify for coverage from Medicare Part B for durable medical equipment for “use in the home” –
- you must be enrolled in Medicare Part B
- you have a signed prescription from a Medicare-enrolled doctor which states that the equipment is a “medically necessary”
- you have to purchase, or to rent, the equipment through a Medicare-enrolled supplier
What counts as “living at home” for Medicare –
- living in your own home
- living in the family home
- living in the community, such as assisted living
Medicare-enrolled DME supplier near me
You can use this link to find a Medicare-enrolled supplier who is local to you – Medicare.gov
What about Medicare Advantage?
Medicare Advantage, or Medicare Part C, are provided by private companies which are contracted by Medicare to provide at least the same services, and coverage, as Original Medicare Parts A and B, and some extra benefits, which Medicare allows them to offer.
This means that Medicare Advantage, or Medicare Part C, will cover Therapeutic shoes and inserts under the same guidelines as Original Medicare.
Each Advantage plan has its network of providers and suppliers, and these will be the only ones you are allowed to use if you are to receive coverage.
List of durable medical equipment covered by Medicare
If you don’t find the equipment you are looking for in my list of Medicare covered DME’s below, you can use this link to Medicare.gov
Air-Fluidized Bed
Alternating Pressure Pads and Mattresses
Audible/visible Signal Pacemaker Monitor
Pressure reducing beds, mattresses, and mattress overlays used to prevent bed sores
Bead Bed
Bed Side Rails
Bed Trapeze – covered if your loved one is confined to their bed and needs one to change position
Blood sugar monitors
Blood sugar (glucose) test strips
Canes (however, white canes for the blind aren’t covered)
Commode chairs
Continuous passive motion (CPM) machines
Continuous Positive Pressure Airway Devices, Accessories and Therapy
Crutches
Cushion Lift Power Seat
Defibrillators
Diabetic Strips
Digital Electronic Pacemaker
Electric Hospital beds
Gel Flotation Pads and Mattresses
Glucose Control Solutions
Heat Lamps
Hospital beds
Hydraulic Lift
Infusion pumps and supplies (when necessary to administer certain drugs)
IPPB Machines
Iron Lung
Lymphedema Pumps
Manual wheelchairs and power mobility devices (power wheelchairs or scooters needed for use inside the home)
Mattress
Medical Oxygen
Mobile Geriatric Chair
Motorized Wheelchairs
Muscle Stimulators
Nebulizers and some nebulizer medications (if reasonable and necessary)
Oxygen equipment and accessories
Patient lifts (a medical device used to lift you from a bed or wheelchair)
Oxygen Tents
Patient Lifts
Percussors
Postural Drainage Boards
Quad-Canes
Respirators
Rolling Chairs
Safety Roller
Seat Lift
Self-Contained Pacemaker Monitor
Sleep apnea and Continuous Positive Airway Pressure (CPAP) devices and accessories
Sitz Bath
Steam Packs
Suction pumps
Traction equipment
Ultraviolet Cabinet
Urinals (autoclavable hospital type)
Vaporizers
Ventilators
Walkers
Whirlpool Bath Equipment – if your loved one is home bound and the pool is medically needed. If your loved one isn’t home bound, Medicare will cover the cost of treatments in a hospital.
Prosthetic and Orthotic Items
Orthopedic shoes only when they’re a necessary part of a leg brace
Arm, leg, back, and neck braces (orthotics), as long as you go to a supplier that’s enrolled in Medicare
Artificial limbs and eyes
Breast prostheses (including a surgical bra) after a mastectomy
Ostomy bags and certain related supplies
Urological supplies
Therapeutic shoes or inserts for people with diabetes who have severe diabetic foot disease.
Free one-on-one help with understanding Medicare
SHIP – State Health Insurance Assistance Programs
There are State Health Insurance Assistance Programs present in all states offering free counseling services on Medicare, Medicaid and Medigap.
I have a post outlining how to find your local SHIP, and how to contact them – “Free Help Understanding Medicare And Medicaid ? Here’s Where You Get It”.
If I don’t have Medicare, what about Medicaid ?
Medicaid programs are funded both federally, and by each individual state.
Consequently, each individual state has quite a lot of room for change with regard to what it does on its Medicaid programs, so long as it stays within the Medicaid guidelines.
In the case of Therapeutic shoes and inserts, you don’t have to worry, as Medicaid covers them if you are eligible for Medicaid.
If you have Medicaid to qualify for the Diabetic shoes and inserts you must be diagnosed with diabetes and, as with Medicare, have one of the following foot conditions –
- history of foot amputation
- history of foot ulcers
- history of pre-ulcer callus
- peripheral neuropathy with evidence of callus
- foot deformity
- poor circulation
Care in the home – Medicaid and state programs
Programs which are primarily for low income families, the disabled and the elderly, and which serve to help the participants maintain their independence, with care in the home, are called “Home and Community Based Services” (HCBS), “Waivers” or “1915 Waivers”.
HCBS programs, waivers, and 1915 waivers will all help to cover “home medical equipment” for the maintenance of the participants’ independence, and will very often cover it up to 100% of the cost.
To find out about your eligibility for HCBS programs or waivers, you can contact your State Medicaid Agency here.
if you want to find out more in general about HCBS programs or waivers, use the link below –
https://www.medicaid.gov/medicaid/hcbs/authorities/index.html
Medicaid uses the term “home” to mean any of the following –
- their own home
- their family home
- a group home
- an assisted living facility
- a custodial care facility
How to find the HCBS programs, waivers and 1915 waivers in your state
If you would like to know which, if any, Medicaid HCBS waivers and programs for seniors are available in your state, you can check my guide which lists them all by state.
In addition, the Money Follows The Person Programs and PACE Programs (Programs of All-inclusive Care for the Elderly) are included.
The guide is here – “Medicaid Home and Community Based Services Waivers and Programs For Seniors Listed By State”.
How to get therapeutic shoes, inserts and other DME’s with Medicaid and state waivers and HCBS programs ?
This is an outline of the typical process, and it may vary with some DME
Step 1
– the doctor, or therapist, has to provide a medical justification letter, stating that your DME is “medically necessary” – in the case of therapeutic shoes and inserts for diabetics, a Certification for Diabetic Shoes form filled out completely by the physician that treats your diabetes is necessary
Step 2
– Medical records from your doctor which documents one of the following conditions –
- history of foot amputation
- history of foot ulcers
- history of pre-ulcer callus
- peripheral neuropathy with evidence of callus
- foot deformity
- poor circulation
Step 3
– find a Medicaid-approved podiatrist or other qualified healthcare provider to prescribe and fit the shoes and inserts – note that they may also be the supplier
Step 4
– the Medicaid-approved supplier fills out a Prior Approval Application form for Medicaid
Step 5
– the Prior Approval Application is sent to the Medicaid State Office
Step 6
– if you are unsuccessful you will be contacted and given the reasons as to why, as well as advice on how to make an appeal
Step 7
– if approved, you will receive the DME – in the case of the shoes and inserts it will vary a little, as the podiatrist, or healthcare provider, who prescribed the shoes and inserts will also have to do your fitting, so if they are the supplier, once they have approval the shoes will be ordered, and you will return for a fitting when they are ready
– if the person who prescribed the shoes and inserts is not the supplier, you will have to get the shoes from the supplier and take them to the person who gave you the prescription and have them correctly fitted
If your income is a bit too high to qualify for Medicaid
Spend Down Programs
Spend-Down programs are designed by Medicaid to help to reduce a person’s income level, or their income level + asset level, so that they may become eligible for Medicaid coverage, by allowing the deduction of certain expenses.
If you want to learn more I’ve written an article outlining who can qualify for Spend Down, the expenses that are deductible and how you know if you qualify – “What is Spend Down ?”
To find your State Medicaid State Agency
If you just want to talk to, or to email someone, contact your state Medicaid Agency here.
Step 1 –
Click the link to Medicaid.gov, look to the section I outlined in red.
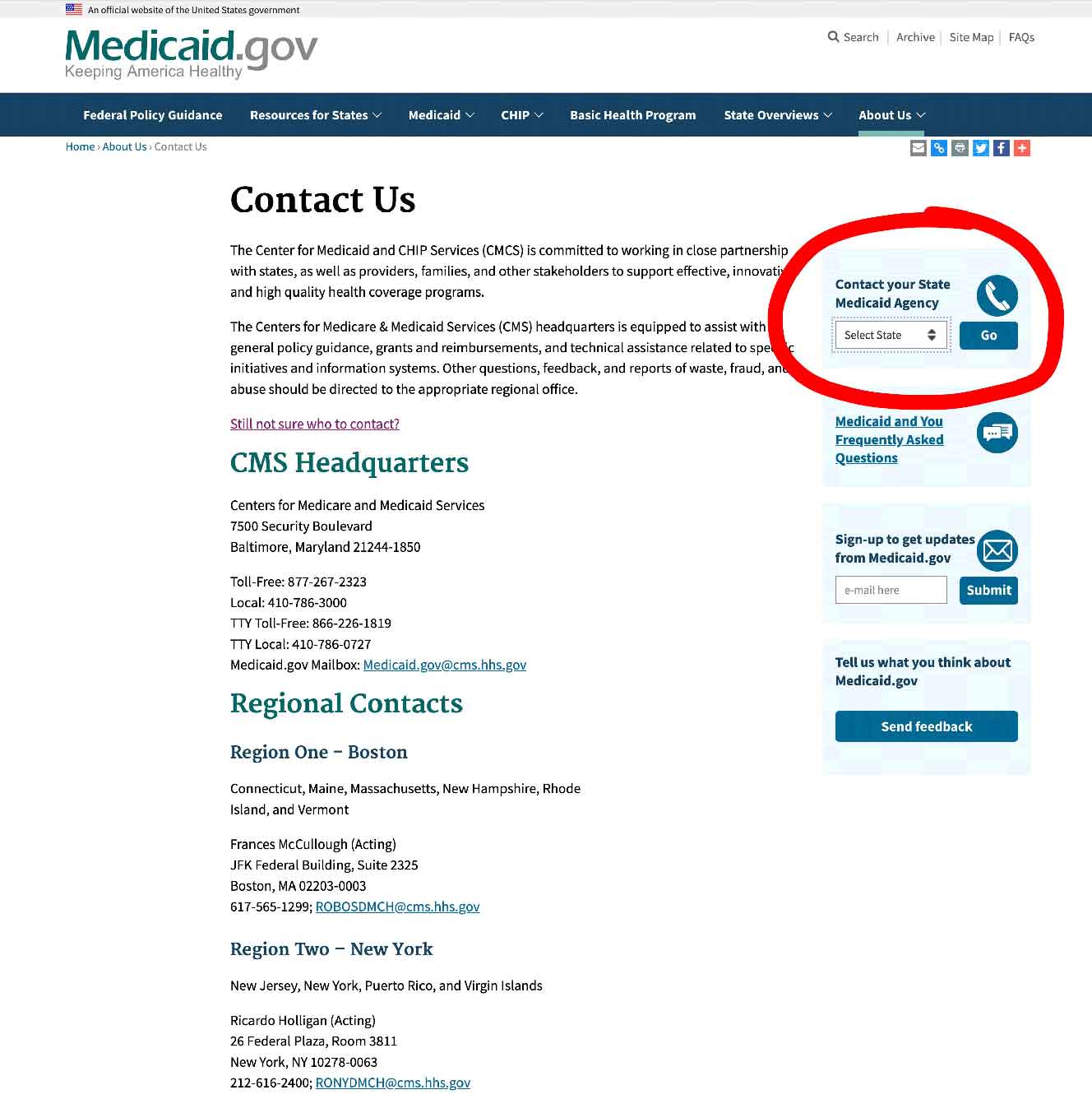
Step 2 –
Select your state and click on the button they have marked “GO” – it will take you to your State Medicaid Agency with all their contact info.
Does Tricare cover therapeutic shoes and inserts for Veterans ?
Tricare covers therapeutic shoes and inserts for diabetes for veterans –
Shoe and insert coverage is limited to one of the following within a calendar year:
- One pair of custom molded shoes (including inserts that come with the shoes) and two pairs of multidensity inserts, or
- One pair of extra-depth shoes (not including inserts that come with the shoes) and three pairs of multidensity inserts.
- You can substitute one of your inserts to modify your custom molded or extra-depth shoes. The most common modifications are:
- Rigid rocker bottoms
- Roller bottoms
- Metatarsal bars
- Wedges
- Offset heels
The text above is from the Tricare website, and you can find it here.
Does ChampVA cover therapeutic shoes and inserts for veterans ?
ChampVa covers –
“For individuals with diabetes, extra-depth shoes with inserts or custom molded shoes with inserts are covered.”
The text is from ChampVA Operational Policy Manual, Chapter 2, Section 17.4, Part IV Policy, Part B on orthotics, and you can check that here.
I’m Gareth, the author and owner of Looking After Mom and Dad.com
I have been a caregiver for over 10 yrs and share all my tips here.

