With so many elderly loved one’s suffering from illnesses related to surplus weight, scales are very important devices to help our loved ones monitor any weight gains or losses. And as with all other pieces of equipment that we need for them, we have to ask the inevitable question….
Does Medicare cover scales ? No, Original Medicare Part B does not cover scales for “use in the home”, as they are not an item which it considers to be “medically necessary” or “primarily medical in nature”.
Contents Overview & Quicklinks
Do Medicare Advantage Plans cover scales ?
Does Medicare cover bathroom equipment ?
Does Medicare cover exercise equipment ?
Does Medicare cover a walking boot ?
How often does Medicare pay for a walker, or other equipment ?
What equipment does Original Medicare cover ?
What is DME ? Durable Medical Equipment definition
Medicare and Durable Medical Equipment
Durable Medical Equipment, which Medicare typically covers
What DME is not covered by Medicare ?
Locate a Medicare-enrolled DME Supplier near you ?
Medicare DME documentation requirements
How does a person qualify for Medicare coverage ?
What do you do with your prescription from your Medicare-enrolled doctor ?
Get free assistance with understanding Medicare
List of Durable Medical Equipment covered by Medicaid
Certain Medicaid and state programs and waivers, which allow for a wider range of DME
How to find the HCBS programs, waivers and 1915 waivers in your state ?
How do you get DME with Medicaid and state waivers and HCBS programs ?
Do Medicare Advantage Plans cover scales ?
If you have a Medicare Advantage Plan, you are covered for everything that Original Medicare Parts A and B cover. You will have at least the same coverage for DME for “use in the home”, and probably a few more benefits depending on your provider.
There may be extra benefits for –
- hearing aids
- vision aids
- gym classes
- transport for shopping
- equipment for chronic illnesses – air conditioners, bathroom grab bars, raised toilet seats
The process for assuring coverage, and for then purchasing the DME, will vary from provider to provider, as each plan will have its own network of doctors and suppliers that they will want you to use.
Always contact your plan provider before you get any equipment.
Does Medicare cover bathroom equipment ?
You may not have been surprised to discover that Medicare doesn’t cover scales, but I think you may be surprised at how much bathroom safety equipment is not covered by Medicare.
Rather a lot of bathroom equipment that is associated with safety, and with making personal hygiene easier, which you may have thought would be covered by Medicare, is not.
I used to think, before researching Medicare, that the more obvious items such as grab bars, raised toilet seats or shower chairs, or anything in fact associated with creating a safer bathroom environment for our elderly parents, would probably have some kind of coverage ……WRONG !!!
Medicare is not there to help prevent elderly from having accidents in the home.
All that Medicare covers has to be “medically necessary”, and as you will see, if you read to the end, this does differ from other funding sources which are there to provide equipment which helps the elderly with avoiding accidents, or just makes living at home possible.
Medicare, for instance, does not cover any of the following –
- grab bars
- raised toilet seats
- bath lifts
- bath seats
- floor to ceiling poles
- shower chairs
- bath chairs
- transfer seats
- toilet safety frames
Thankfully though, when it is medically necessary for the elderly with mobility problems, Medicare Part B does cover crutches, walkers and bedside commodes, all of which can be very useful in the bathroom.
To get coverage, the equipment must be prescribed by a Medicare-enrolled doctor and be “medically necessary”.
In the case of this type of equipment, it means that the person cannot stand without the aids, and these will necessarily improve their quality of life and help with their condition, especially in the bathroom.
Medicare Advantage Plans, or Medicare Part C, is different with regard with to some newer benefits which have been allowed for individuals with chronic illnesses.
Advantage Plans may now offer benefits which may include some bathroom safety equipment, or even bathroom modifications, for certain chronic illnesses if it relieves the stress on Original Medicare – and these are benefits which are not available on Original Medicare.
I have a long article with 50 plus safety tips that I have learned over the 11 years that I have looked after my mom and dad. These are both practical tips, and some suggestions for equipment you may find helpful. You can read the article here.
If you are looking for suggestions and advice on how to make bathing easier for your parent, especially if you are assisting them, then I have another article. I discuss the ways that I have found to make the bathing a more comfortable, and dignified experience, for all parties – that one is here.
Does Medicare cover exercise equipment ?
Exercise equipment is not considered “medically necessary” by Original Medicare along with, in most cases, exercise classes.
The use of exercise equipment, though, is covered by Original Medicare Part B when it is in treatment sessions with physiotherapy and occupational therapy, where it is prescribed as “medically necessary” by a doctor.
The treatment must be given on an outpatient basis by a Medicare-certified therapist, and the therapy must be under regular review by the prescribing doctor.
As with any medical equipment, you will need to make sure that the therapist charges the Medicare-approved fee for the therapy in question.
If you do everything by the book, Medicare typically covers 80% of the Medicare- approved fee, and the patient covers the 20% of the fee, plus their deductible if it applies.
With a Medicare Advantage plan some have coverage for exercise plans and gyms, but always check with the provider before signing up for anything.
Does Medicare cover a walking boot ?
An example of a piece of equipment which is, in some cases, covered is a “walking boot”.
“Walking Boots” are covered under the benefit for Orthotics or Braces by Medicare Part B, for certain types of boot, and for certain types of treatments only –
- the “walking boot” has to be rigid or semi-rigid
- the treatment it is used for, must be to immobilize the ankle/foot following orthopedic surgery, or for an orthopedic condition
As per all Medicare coverage, it is necessary to have a signed prescription from a Medicare-enrolled physician which says the “walking boot” is “medically necessary”.
Medicare will not give coverage to “walking boots” if they are used to relieve pressure to treat ulcers and foot sores associated with diabetes, or other conditions.
Medicare Part B covers therapeutic shoes and inserts for conditions such as diabetes, but not under the benefit for Orthotics or Braces.
How often does Medicare pay for a walker, or equipment ?
Medicare Part B’s policy is to replace DME that you rent, or own, if they are –
- worn out through use
- have been in your possession for their entire lifetime
- so worn out that they can’t be fixed
- five years is the minimum period considered to be a lifetime for an item
- the lifetime can vary depending on the type of equipment
If you have a worn out walker, Medicare Part B will typically replace it every five years, so long as it has only been yours, and that the walker is beyond repair.
If an item has worn out prior to the end of its lifetime, Medicare will pay to have it repaired, unless it’s the case that the repair is more costly than a replacement.
The process for obtaining the replacement item is the same as the initial process for the first item with coverage – a prescription from a Medicare-enrolled doctor stating that the equipment is medically necessary.
What equipment does Medicare cover ?
Original Medicare Part B covers Durable Medical Equipment, or DME, for use in the home which has been prescribed as “medically necessary”.
If Medicare is going to cover a claim for DME, it must be accompanied by the correct paper work and case documentation.
Medicare Part B does not cover disposable medical equipment unless used specifically in conjunction with a qualifying item of durable medical equipment which is being covered.
Durable Medical Equipment which is used in skilled nursing facilities is covered by Original Medicare Part A.
What is DME ? Durable Medical Equipment definition
Durable Medical Equipment must fulfill the following criteria –
- it must withstand repeated use over a sustained period of time – durable
- it is to be used for medical reasons only – not for comfort
- it’s got to be useful to a person who is sick, and not to those who aren’t
- it is to be used primarily in the home
- it must be expected to last a minimum of 3 years
Medicare and Durable Medical Equipment
It also has to be understood that just because an item of medical equipment falls into the Durable Medical Equipment category, it does not necessarily mean that you can automatically get coverage for it, if you want to have it.
A Medicare-enrolled physician has to prescribe the DME as “medically necessary” for you, and has to provide a Certificate of Medical Necessity, as well as records and documentation which attest to, and support, the diagnosis of your condition.
There is also, in many cases, the need to have had a face-to-face encounter with the prescribing practitioner within six months prior to the date of the sending of the claim.
Durable medical equipment, which Medicare Part B typically covers
If you don’t find the equipment you are looking for in my list of Medicare covered DME below, you can use this link to Medicare.gov
Air-Fluidized Bed
Alternating Pressure Pads and Mattresses
Audible/visible Signal Pacemaker Monitor
Pressure reducing beds, mattresses, and mattress overlays used to prevent bed sores
Bead Bed
Bed Side Rails
Bed Trapeze – covered if your loved one is confined to their bed and needs one to change position
Blood sugar monitors
Blood sugar (glucose) test strips
Canes (however, white canes for the blind aren’t covered)
Commode chairs
Continuous passive motion (CPM) machines
Continuous Positive Pressure Airway Devices, Accessories and Therapy
Crutches
Cushion Lift Power Seat
Defibrillators
Diabetic Strips
Digital Electronic Pacemaker
Electric Hospital beds
Gel Flotation Pads and Mattresses
Glucose Control Solutions
Heat Lamps
Hospital beds
Hydraulic Lift
Infusion pumps and supplies (when necessary to administer certain drugs)
IPPB Machines
Iron Lung
Lymphedema Pumps
Manual wheelchairs and power mobility devices (power wheelchairs or scooters needed for use inside the home)
Mattress
Medical Oxygen
Mobile Geriatric Chair
Motorized Wheelchairs
Muscle Stimulators
Nebulizers and some nebulizer medications (if reasonable and necessary)
Oxygen equipment and accessories
Patient lifts (a medical device used to lift you from a bed or wheelchair)
Oxygen Tents
Patient Lifts
Percussors
Postural Drainage Boards
Quad-Canes
Respirators
Rolling Chairs
Safety Roller
Seat Lift
Self-Contained Pacemaker Monitor
Sleep apnea and Continuous Positive Airway Pressure (CPAP) devices and accessories
Sitz Bath
Steam Packs
Suction pumps
Traction equipment
Ultraviolet Cabinet
Urinals (autoclavable hospital type)
Vaporizers
Ventilators
Walkers
Whirlpool Bath Equipment – if your loved one is home bound and the pool is medically needed. If your loved one isn’t home bound, Medicare will cover the cost of treatments in a hospital.
Prosthetic and Orthotic Items
Orthopedic shoes only when they’re a necessary part of a leg brace
Arm, leg, back, and neck braces (orthotics), as long as you go to a supplier that’s enrolled in Medicare
Artificial limbs and eyes
Breast prostheses (including a surgical bra) after a mastectomy
Ostomy bags and certain related supplies
Urological supplies
Therapeutic shoes or inserts for people with diabetes who have severe diabetic foot disease.
What DME is not typically covered by Medicare ?
Adult Diapers
Air Cleaners
Air Conditioners
Alcohol Swabs
Augmentative Communication Device
Bathroom Aids
Bathtub Lifts
Bathtub Seats
Bed Bath
Bed Boards
Bed Exit Alarms
Bed Sensor Pads
Bed Lifter
Beds – Lounge
Bed Wedges
Blood Glucose Analyzers
Braille Teaching Texts
Caregiver Paging Systems
Catheters – except those which are used for permanent medical conditions where the catheter is considered as a prosthetic
Chair Exit Alarms
Chair Sensor Pads
Communicator
Contact Lenses – Medicare helps pay for corrective lenses if you have cataract surgery to implant an intraocular lens
Dehumidifiers
Dentures
Diathermy Machines
Disposable Bed Protectors
Disposable Sheets
Door Exit Alarms
Easygrip Scissors
Elastic Stockings
Electrical Wound Stimulation
Electrostatic Machines
Elevators
Emesis Basins
Esophageal Dilators
Exercise Machines
Exit Alarm Mat
Eyeglasses – Medicare helps pay for corrective lenses if you have cataract surgery to implant an intraocular lens.
Fall Alarms
Fans
Fabric Supports
Fomentation Device
Grab Bars
Grabbers
Gauze
Hearing Aids
Heat and Massage Foam Cushion Pad
Heating and Cooling Plants
Home Modifications
Humidifiers – not room humidifiers
Incontinence Pads
Injectors (hypodermic jet pressure powered devices for Insulin injection)
Irrigating Kits
Insulin Pens
Massage Equipment
Motion Sensors
Motion Sensor Exit Systems with Pagers
Needles
Oscillating Beds
Over bed Tables
Paraffin Bath Units (if not Portable)
Parallel Bars
Portable Room Heaters
Portable Whirlpool Pumps
Preset Portable Oxygen Units
Pressure Leotards
Pressure Stockings
Pulse Tachometer
Pull String Alarms
Raised Toilet Seats
Ramps
Reading Machines
Reflectance Colorimeters
Sauna Baths
Special TV Close Caption
Speech Teaching Machines
Stair Lifts
Standing Table
Support Hose
Surgical Face Masks
Surgical Leggings
Syringes
Telephone Alert Systems
Television Assistive Listening Devices
Telephone Arms
Toilet Seats
Treadmill Exercisers
Walk in Bathtubs
Wheelchair Lifts
Whirlpool Pumps
White Canes
Wigs
Find a Medicare-enrolled DME Supplier near you
To find a local Medicare supplier, check this here at Medicare.gov
Medicare DME documentation requirements
Medicare may require any parts of the beneficiary’s medical records pertaining to the history of the condition, physical examinations, diagnostic tests, summary of findings, diagnoses, treatment plans, which support the medical necessity of the DME and statements of the anticipated benefits and outcomes.
This record need not be limited to the office records of the physician, it can include records from nursing homes, hospitals, home health agencies, and other health care professionals.
This has to accompany the Certificate of Medical Necessity, which by itself is does not provide sufficient documentation of medical necessity.
A valid written order prior to delivery is required for certain items such as hospital beds.
Sources –
https://wisequestion.com/durable-medical-equipment-medicare-documentation/
https://www.compliance.com/resources/durable-medical-equipment-dme-documentation-required-for-medicare-payment/
https://www.cms.gov/Regulations-and-Guidance/Guidance/Manuals/downloads/pim83c05.pdf
Medicare free supplies
Medicare Part B does not cover medical supplies, because they are disposable items.
The only exception to this, are disposable supplies which are needed for use with this durable medical equipment, and blood sugar strips and certain catheters which may be covered by Medicare, if they are needed for use in conjunction with durable medical equipment, and, or, to treat long term medical conditions.
Medicare doesn’t cover any of the following supplies – diapers, bandages, face masks, elastic stockings, pressure leotards, support hose, surgical leggings, disposable sheets and bags, fabric supports and incontinence pads.
These items are disposable and not durable, and are not used in conjunction with a piece of durable medical equipment.
If you are receiving Home Health Care, Medicare will cover some supplies needed for your care under the Home Health Care Benefit.
How does a person qualify for Medicare coverage ?
To get coverage of DME “for use in the home” with Original Medicare Part B, you –
- must be enrolled in Medicare Part B
- need a signed prescription from your Medicare-enrolled doctor saying that the DME is “medically necessary”
- have to go through a supplier who is a Medicare-enrolled supplier
To qualify for DME for “home use” –
You must be –
- living in your own home
- living in the family home
- living in the community, such as assisted living
What do you do with your prescription from your Medicare-enrolled doctor ?
With the prescription in hand, you should do the following –
- locate a Medicare-enrolled DME supplier who has your type of DME
- make sure the supplier is a Medicare-enrolled “participating” supplier who accepts “assignment” – this ensures you don’t pay any surplus
- although the equipment Medicare gives coverage is only the basic models, you can, in certain cases, if you pay extra, get upgrades
- select the example you want of the DME from those you have been prescribed
- complete all the necessary paperwork with the supplier, in compliance with any Medicare rules
If you have used a Medicare-enrolled supplier and your prescription is from a Medicare-enrolled doctor stating that your DME is “medically necessary”, Medicare part B will cover 80% of the Medicare-approved price for DME.
If you have used a Medicare-enrolled “Participating” supplier who accepts “assignment”, you’ll only pay your Medicare 20% co-payment of the Medicare-approved price for the DME, as well as your deductible if it applies.
Always purchase or rent from a Medicare-enrolled supplier who is a Medicare-enrolled “Participating” supplier who accepts “assignment”, as they have accepted to charge just the Medicare-approved price for equipment.
If a Medicare-enrolled supplier is not a “Participating” supplier who accepts “assignment”, it means that the supplier can add up to 13% to the Medicare-approved price for the equipment, and it will be paid by you, and not by Medicare.
Medicare may rent or purchase your DME – in cases where Medicare decides to rent the DME, rather than purchasing it, you will have the same payment structure as for purchased equipment – you will simply pay a monthly 20% co-payment of the monthly rental fee, plus a one time payment of your deductible, if it applies.
Get free assistance with understanding Medicare
SHIP – State Health Insurance Assistance Programs
For anyone needing guidance with Medicare, Medicaid and Medigap, you can get it for free over the phone from State Health Insurance programs throughout the US
All SHIPs offer free counseling services.
If you need help to find your SHIP, you can go to my short guide on how to find and contact your SHIP here – “Free Help Understanding Medicare And Medicaid ? Here’s Where You Get It”.
List of Durable Medical Equipment covered by Medicaid ?
There is no definitive list of Durable Medical Equipment covered by Medicaid, as Medicaid is administered on both a federal and a state level, so there is not one set of rules and equipment covered.
There are hundreds of Medicaid and state programs and waivers across the US, with varying rules for eligibility, and interpretations of what equipment qualifies as Durable Medical Equipment.
Typically, for Medicaid, Durable Medical Equipment must –
- be medically necessary, as determined by a medical physician or treating practitioner
- meet the standard definition of “Durable Medical Equipment” for the CMS (Centers for Medicare and Medicaid Services)
Durable Medical Equipment is defined as –
- the equipment must be able to withstand repeated use over a sustained period of time
- the equipment must be used for a medical purpose only
- the equipment is for use in the home, first and foremost
- the equipment is not useful to a person who is not ill or injured
But as I said above, depending on the different programs and waivers, what is qualifies as DME will vary
Will Medicaid cover scales ?
Medicaid will often allow states to waive certain of the eligibility criteria for various programs, so that different groups of people, who may otherwise have been missed, will instead qualify and receive health care.
These programs are then called waivers.
Each waiver will have its own eligibility criteria, in order that it may help a specific group of people.
Care in the home – Medicare and state programs
The programs which are specifically for care in the home and the community are called – “Home and Community Based Services” (HCBS), “Waivers” or “1915 Waivers”
The goal of these programs is to help the beneficiaries to maintain their independence, and to remain living in their own homes, and the community.
These programs are for low income families, disabled individuals and the elderly.
If you contact your State Medicaid Agency, you can find out if you are eligible here.
You can also ask at your local Area Agency on Aging about waivers for the elderly in your state.
To learn more about HCBS programs, or waivers, use the link below –
https://www.medicaid.gov/medicaid/hcbs/authorities/index.html
To avoid unnecessarily placing the elderly and the disabled in state care facilities, and to keep them in their own homes, the HCBS programs, waivers and 1915 waivers, cover a wide range of home medical equipment, and will often cover 100% of the costs.
For the purposes of the HCBS programs, waivers and 1915 waivers, any of the following situations qualify as a “home” –
- their own home
- their family home
- a group home
- an assisted living facility
- a custodial care facility
Certain Medicaid and state programs and waivers, which allow for a wider range of DME
Some HCBS waivers, programs, and 1915 waivers allow for “Consumer Direction” or “Self Direction”.
Each program participant will be given a budget.
The program participant is very much responsible for how the budget is spent, with the help of an appointed a financial advisor they will decide what is necessary.
These programs and waivers exist so that the participants can stay living in their own homes, so if certain equipment is necessary for them to remain independent, and the budget can cover it, they will very frequently be allowed to get it.
What can be bought as DME here is far less restricted than with Medicare, as necessity, pretty much, defines what is and isn’t allowed.
You can read more about Medicaid Self Direction here.
Transitioning the elderly out of care facilities back into their homes
Money follows the person – is a Medicaid based program which helps to return elderly adults to their homes after they have been in state care facilities, so that, if they are able, they can regain their independence.
Assisted living also counts as an individual’s own home for this program.
If DME are needed for the transition they are purchased by the program – this can go as far as remodeling the bathroom, or kitchen, if it is necessary for the move to take place.
How to find the HCBS programs, waivers and 1915 waivers in your state
If you would like to find Medicaid HCBS waivers and programs for seniors in your state, you can check my guide which lists them by state, as well as the Money Follows The Person Programs and PACE Programs (Programs of All-inclusive Care for the Elderly). You can find the guide here – “Medicaid Home and Community Based Services Waivers and Programs For Seniors Listed By State”.
How do you get DME with Medicaid and state waivers and HCBS programs ?
Step 1
– get a medical justification letter from your doctor, or therapist, which states that the equipment is medically necessary
Step 2
– find a Medicaid-approved DME supplier and give to them the medical justification letter
Step 3
– the DME supplier should fill out a Prior Approval Application for Medicaid
Step 4
– the application is then sent to the Medicaid State Office
Step 5
– if your application is unsuccessful you will be notified as to the reasons why, and given advice on how to appeal the decision
Step 6
– if approved, you will receive the DME you applied for
If you don’t quite qualify for Medicaid
Spend Down Programs
If you find that you are above the Medicaid income limit, or income + asset limit, and not eligible for coverage, you may still be eligible for a Spend Down Program.
“Spending Down” is the name of the method used by Medicaid to help to reduce a person’s income level in just that situation.
“Spending Down” involves deducting certain expenses from a person’s income.
To learn more about Spend Down you can read my post about who can qualify for Spend Down, which expenses are deductible and how to find out if you qualify – “What is Spend Down ?”
How to find your State Medicaid State Agency
You can also contact your state Medicaid Agency, and you can do that here.
Step 1 – Once you have clicked the link to Medicaid.gov, look at the section I have outlined in the image below
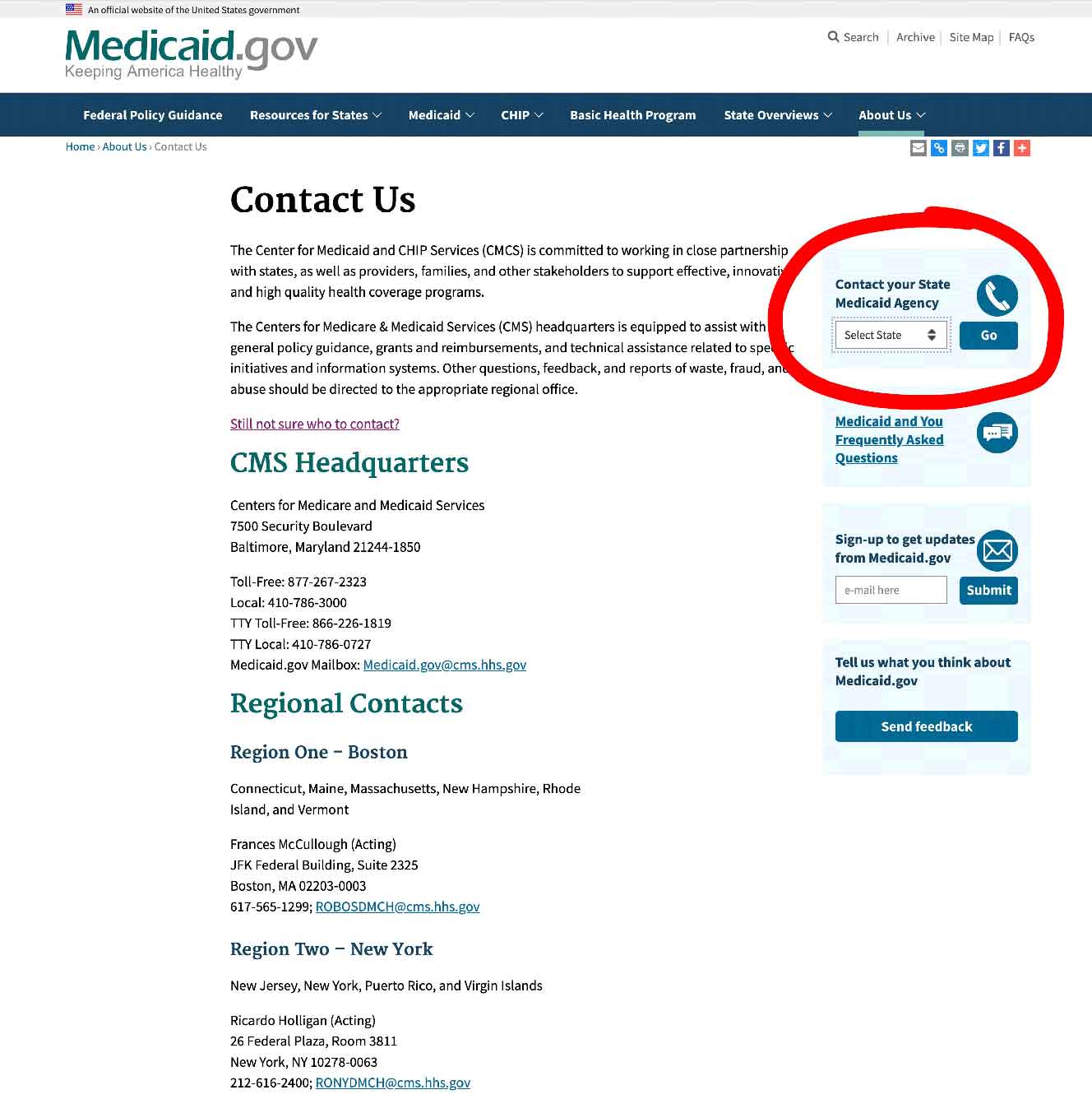
Step 2 – select your state, and click on “GO” – it will take you to your State medicaid Agency.
State Funding Assistance
Assistive Technology Programs
Each state has its own Assistive Technology Programs to increase access to assistive devices – the primary focus is on the elderly and the disabled.
These assistive devices include DME and any equipment which enables a person to complete tasks they otherwise cannot complete – this can range from grab bars to electronic digital devices.
To find out what programs your state runs, click here.
Step 1/
Select your state on the map or from the drop-down menu and click on the button “Go to state”
– I chose Florida for this example
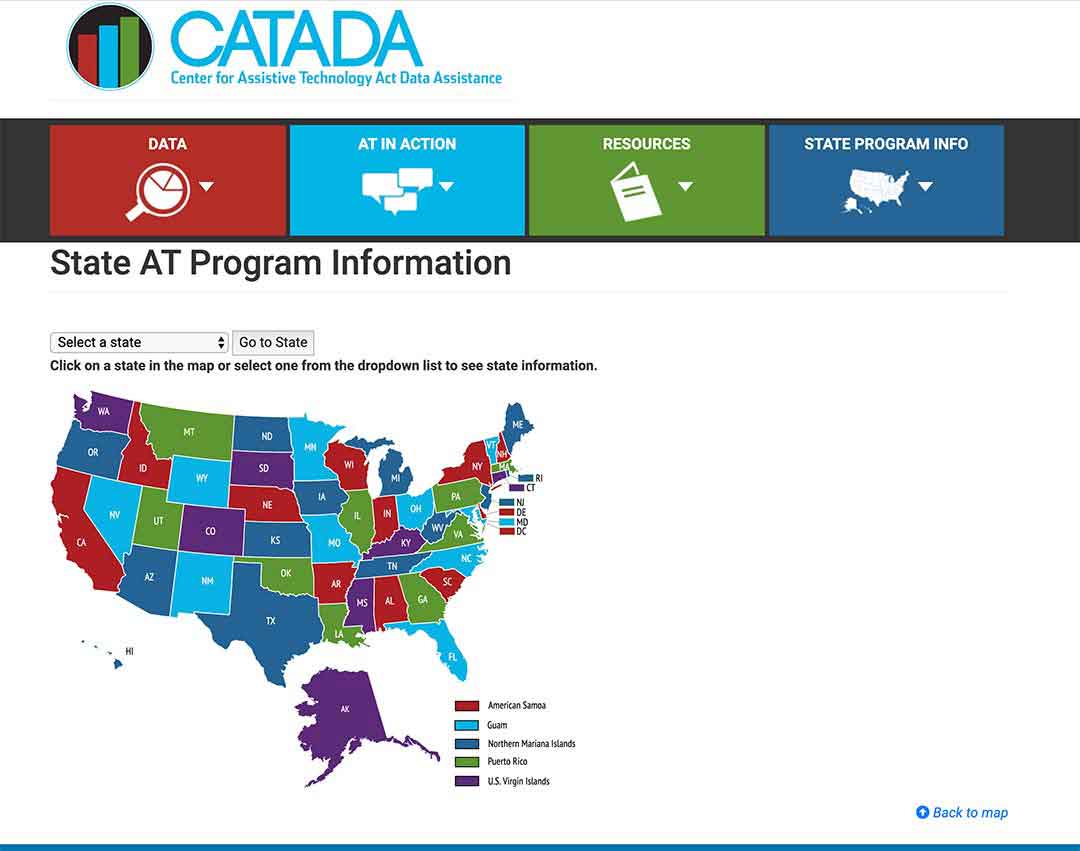
Step 2/
Look for the link “Program Title” – for my example I outlined it in red – and click on that.
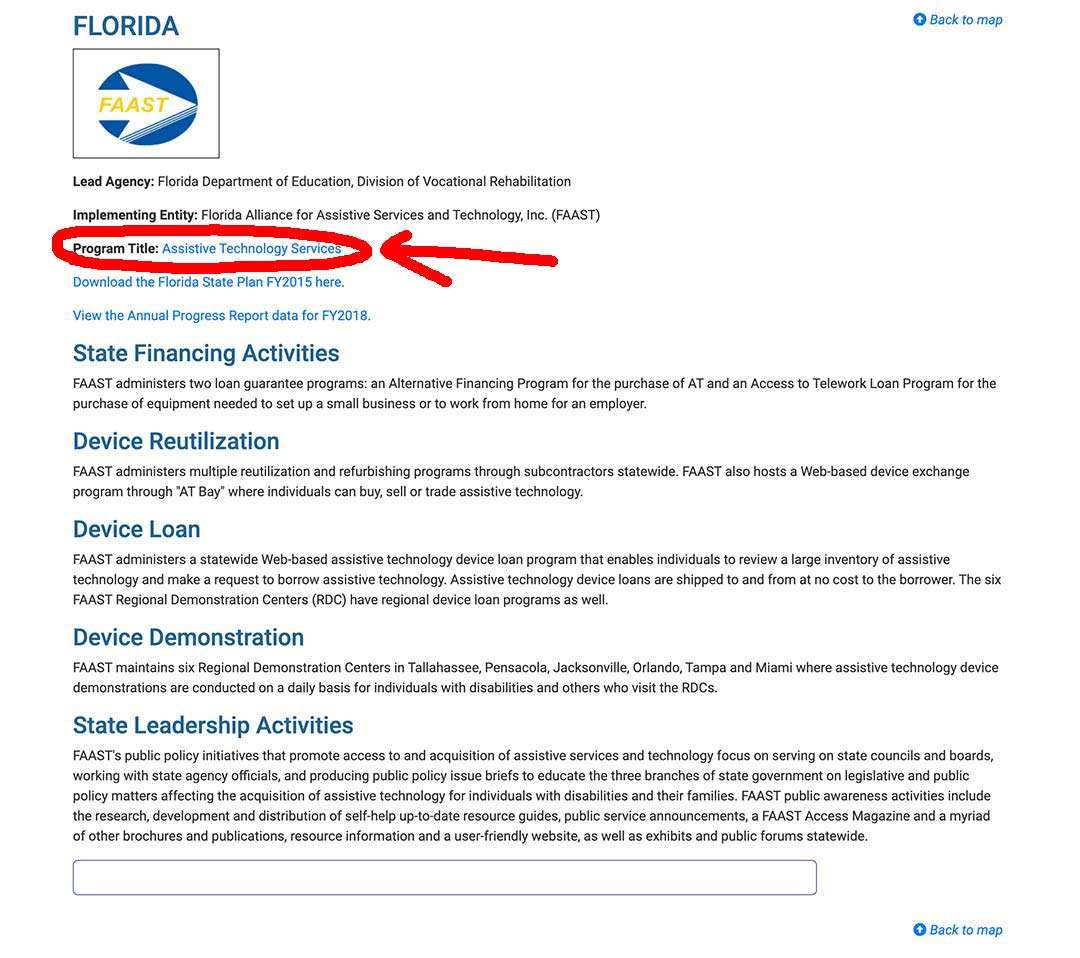
Step 3/
The State AT Program website will come up, and you can
- sign up
- use their contact info to get in touch
- find out what they offer to help the elderly
- find out if you, or a loved one, are eligible
State Financial Assistance Programs
These are state non-Medicaid programs which provide assistance so that the elderly and the disabled so that they may remain living in their homes.
The program’s participants get safety equipment and assistive devices, paid for with grants, loans, or a combination of both.
The programs will even cover the costs of remodeling bathrooms, wheelchair ramps and kitchen modifications – all to keep the elderly and disabled participants from being unnecessarily institutionalized.
The primary focus of these programs is on the elderly and the disabled.
Contact your local Area Agency on Aging to help you find the programs in your area, and to determine whether you are eligible to participate.
I’m Gareth, the author and owner of Looking After Mom and Dad.com
I have been a caregiver for over 10 yrs and share all my tips here.

